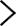Keratoconus is an eye condition that occurs when the cornea (the clear front part of the eye) progressively becomes thinner and begins to bulge out in a cone-like shape. The cornea plays an important part in focusing light onto your retina. Therefore, even minor changes can affect visual clarity. As keratoconus progresses, it may cause the vision to become blurred, distorted or uneven. Let’s learn about the symptoms, causes, treatments and more.
What are the symptoms of keratoconus?
In the early stages, keratoconus often appears to be a normal change in your vision. You may just think you need a new prescription. But as the shape of your cornea continues to change, you will notice more vision problems, such as:
- Blurred and distorted vision
- Light sensitivity
- Halos and glare around lights, especially at night
- Frequent changes in prescription
- Difficulty seeing in the dark
- Noticeable difference in vision between both eyes
As most of the visual changes related to keratoconus happen over an extended period, many people adapt to these changes without recognising that they have a problem. This makes it more important to get eye exams regularly for timely diagnosis and treatment.
Causes of keratoconus
The exact cause for keratoconus is still uncertain. However, research shows that it results from a combination of genetic and environmental factors. In addition to that, several risk factors are also linked to the risk of keratoconus, such as:
- Family history of keratoconus
- Frequent or repetitive rubbing of the eyes
- Allergies that cause itchy eyes
- Connective tissue disorders
- Asthma, eczema or hay fever
How is keratoconus diagnosed?
Keratoconus is diagnosed via comprehensive eye exams that evaluate the shape and the thickness of your cornea. In some cases, an optician may initially suspect keratoconus if frequent changes to your prescription or sudden distortion to your vision have occurred.
To confirm the diagnosis of keratoconus, additional specialised testing is usually performed. These tests can include:
- Corneal topography - This is one of the most important tests to confirm the diagnosis of keratoconus. Corneal topography maps the surface of the cornea with detail, allowing detection of any abnormal shape change.
- Pachymetry - This test measures the thickness of your cornea, so areas that may be thinning can be identified.
- Slit-lamp examination - This visualises the front of your eye under magnification and allows the optician to visually evaluate for signs of keratoconus.
- Refraction tests - These tests evaluate how your vision is changing over time and help determining the appropriate prescription you need.
By identifying keratoconus at an early stage, treatment can help slow the progression and improve long-term outcomes. After a definitive diagnosis, the treatment is aimed at improving vision and preventing further deterioration of your vision.
Keratoconus treatment options
Treatment for keratoconus depends on how severe the condition is at the time of diagnosis. Keratoconus currently has no cure, but there are modern treatments that can help improve your vision or slow down progression of the condition.
Treatment in early stages of keratoconus
During the early stage, patients may only need to correct their vision through the use of regular glasses or contact lenses. But, as the condition continues to progress, the use of special contact lenses may provide more precise and stable visual acuity, such as rigid gas permeable, hybrid and scleral lenses. These lenses are intended to create a smoother optical surface over the eye, allowing light to focus correctly on the retina despite changes in the shape of the cornea.
Treatment in the progressive stage
When the condition progresses, the most common procedure recommended is corneal crosslinking. It is an effective treatment that’s widely used for slowing or halting the progression of keratoconus. Corneal crosslinking consists of putting riboflavin eye drops in the eye and using UV-A light in a controlled manner to strengthen the corneal tissue. It is important to note that this treatment does not reverse any existing corneal distortion but can help prevent or slow down the progression of any additional corneal distortion.
Treatment in the advanced stage
If contact lenses cannot correct your vision any longer, surgical options may be recommended. This includes implantation of intracorneal ring segments (ICRS) for improving the shape of the cornea for better visual focus. A corneal transplantation may be considered if your vision is significantly affected by advanced keratoconus.
Frequently asked questions
Can keratoconus cause blindness?
Keratoconus rarely causes blindness but if left untreated, there are chances of significant visual impairment. With proper care using modern techniques and tools, most patients will maintain sufficient visual acuity.
How fast does keratoconus progress?
It differs for everyone. Some individuals experience very slow vision changes over long periods, while others may experience rapid progression. Regular checkups are the best way to keep track of your keratoconus.
What is the best keratoconus treatment?
To get the best keratoconus treatment based on how advanced the eye condition is, it is highly recommended that you discuss with your eye care professional. For early stages, you may only require glasses or contact lenses; however, there are other treatments you could use depending on the progression of the condition (mild, moderate or severe).
Disclaimer: The advice in this article is for informational purposes only and does not replace medical care or an in-person check-up. Please check with an eyecare professional before purchasing any products or remedies. For information on our article review process, please refer to our Editorial Policy.

 Offers
Offers Account
Account
 Favorite
Favorite
 Basket
Basket

 OFFERS
OFFERS